Expand all
Collapse all
Overview
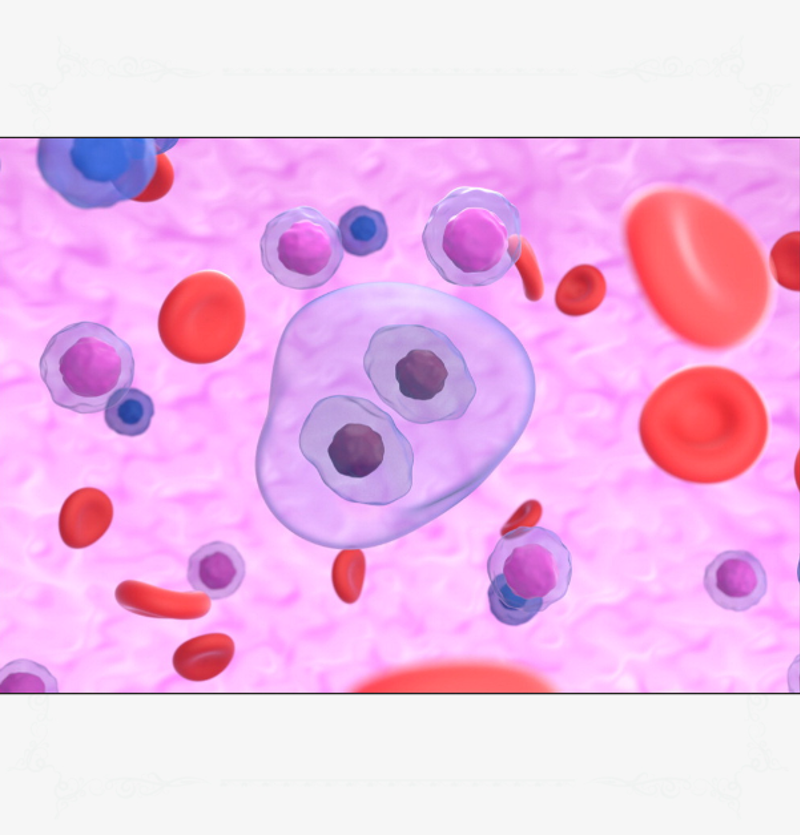
Hodgkin lymphoma has four classified subtypes and is diagnosed by the confirmed presence of Reed-Sternberg cells (Moffitt Cancer Centre, 2018). Kuppers and Hansmann (2005) described these cells as large, multinucleated cells with strange morphology and a phenotype that does not represent any normal body tissue (Figure 1). This disease originates only from the B lymphocyte cells and its four subtypes include (DeVita et al, 2015):
- classic
- nodular
- lymphocyte depleted
- lymphocyte rich.
Non-Hodgkin lymphoma by contrast has 60 different classified subtypes, including follicular, mantle cell and Burkitt lymphoma (DeVita et al, 2015) (Figure 2). These subtypes can be categorised into two groups: aggressive (60%) and indolent (40%).
To view the rest of this content login below; or read sample articles.
Symptoms
A universal principle in predicting the outcome of a cancer is that the earlier a diagnosis is made the better the prognosis. Both these disease profiles conform to this principle and it is at diagnosis that the first main similarities between the two are observed. De Vita et al's (2016) list of presenting symptoms specific to lymphomas are grouped under the umbrella term ‘B symptoms’, with or without the presence of a palpable lump, which are:
- fever
- weight loss
- night sweats.
The presence of B symptoms, as defined by Lymphoma Action (2021a), suggests the likelihood of a worse prognosis in both patient groups compared with those presenting with a palpable lump or pain caused by an internal mass in isolation. Other presenting symptoms of the lymphoma patient are less well defined, and may include indigestion, pain, repeated infection, unexpected bruising or bleeding. Although not specific to lymphoma, if a patient who
To view the rest of this content login below; or read sample articles.
Diagnosis
Both patient Hodgkin lymphoma and non-Hodgkin lymphoma groups are diagnosed by lymph node biopsy, followed by a further biopsy of bone marrow, to confirm a positive diagnosis. Lymph node biopsy may require a general anaesthetic, depending on the accessibility of the mass (NHS website, 2020). Radiological imaging is used to establish the extent of the disease, most commonly, initially by CT scan, followed by a PET scan.
Staging
The disease is staged using the Ann Arbor system (Shankland et al, 2012) (Table 2). The patient will be diagnosed with disease stage I-IV (1-4), depending on the number and location of lymph nodes and other structures involved at diagnosis and then designated as A/B, depending on the absence or presence of other symptoms (Table 2).
| Stage I | Involvement of a single lymph node region or of a single extra organ or site |
| Stage II: | Involvement |
To view the rest of this content login below; or read sample articles.
Treatment
The key aim of treatment for Hodgkin lymphoma and non-Hodgkin lymphoma is remission, which the National Cancer Institute (2017) defines as an absence of signs or symptoms in a patient with a diagnosed malignancy that cannot be surgically removed.
Hodgkin lymphoma
Hodgkin lymphoma patients will be offered treatment with combination chemotherapy, most commonly with a regimen that is abbreviated to ABVD, which includes doxorubicin, bleomycin, vinblastine and dacarbazine (Macmillan Cancer Support, 2021a) (Table 1). These drugs are administered in 28-day cycles, with all drugs given on days 1 and 15, along with a number of supportive medications tailored to individual patient need. The combination therapy will be administered for 2–6 cycles, depending on disease staging. At each treatment interval patients are assessed for fitness for treatment using the National Cancer Institute (2019) common toxicity criteria for adverse events, alongside an evaluation of up-to-date blood tests and a patient's emotional
To view the rest of this content login below; or read sample articles.
Resources
References
Ahmadzadeh A, Yekaninejad MS, Jalili MH et al. Evaluating the survival rate and the secondary malignancies after treating Hodgkin’s lymphoma patients with chemotherapy regimens. Int J Haemat Oncol Stem Cell Res. 2014;8(2):21–26.
American Cancer Society. Key statistics for Hodgkin lymphoma. 2021. https://www.cancer.org/cancer/hodgkin-lymphoma/about/key-statistics.html (accessed 14 December 2022)
Bond DA, Maddocks KJ. Current role and emerging evidence for bruton tyrosine kinase inhibitors in the treatment of mantle cell lymphoma. Hematol Oncol Clin North Am. 2020;34(5):903-921. https://doi.org/10.1016/j.hoc.2020.06.007
Cancer Research UK. Hodgkin lymphoma statistics: Hodgkin lymphoma incidence. 2021a. https://www.cancerresearchuk.org/health-professional/cancer-statistics/statistics-by-cancer-type/hodgkin-lymphoma#heading-Zero (accessed 14 December 2022)
Cancer Research UK. Non-Hodgkin lymphoma statistics: Non-Hodgkin lymphoma (NHL) incidence. 2021b. https://www.cancerresearchuk.org/health-professional/cancer-statistics/statistics-by-cancer-type/non-hodgkin-lymphoma#heading-Zero (accessed 14 December 2022)
Cancer Research UK. Hodgkin lymphoma statistics: Hodgkin lymphoma incidence: Hodgkin lymphoma incidence by sex and by country. 2021c. https://www.cancerresearchuk.org/health-professional/cancer-statistics/statistics-by-cancer-type/hodgkin-lymphoma/incidence#heading-Zero (accessed 14 December 2022)
Cancer Research UK. Hodgkin lymphoma statistics: Hodgkin lymphoma incidence: Hodgkin lymphoma incidence by age. 2021d. https://www.cancerresearchuk.org/health-professional/cancer-statistics/statistics-by-cancer-type/hodgkin-lymphoma/incidence#heading-One (accessed 14 December 2022)
Cancer
To view the rest of this content login below; or read sample articles.